Breadcrumb
- Home
- Conditions & Treatments
- Deep Brain Stimulation
The Movement Disorders Program at Boston Children’s Hospital provides specialized, multidisciplinary care for children with dystonia and other rare, complex movement disorders. As part of this care, we offer deep brain stimulation (DBS), a surgical treatment that can help improve symptoms, comfort, and quality of life. DBS may be recommended for certain genetic forms of dystonia and for children whose symptoms don’t improve with medication alone or significantly interfere with daily activities and require care from multiple specialists.
Our pediatric DBS team brings together experts in neurology, neurosurgery, genetics, rehabilitation, and other specialties to carefully evaluate each patient and support families through every stage of care — from the first consultation through long-term follow-up.
What is deep brain stimulation?
Deep brain stimulation (DBS) is a surgical treatment that uses gentle electrical signals to regulate abnormal brain activity that causes involuntary movement. In some children with movement disorders, faulty brain circuits send excessive signals to the muscles, leading to stiffness, unusual postures, and difficulty moving. DBS delivers adjustable stimulation to specific areas of the brain to calm these signals and reduce symptoms. While not a cure, DBS can significantly improve symptoms and quality of life for some children.
Benefits of DBS may include:
- Fewer uncontrollable movements
- Improved posture, mobility, and coordination
- Reduced pain related to dystonia
- Greater independence in daily activities
- Improved ease of daily care
- Ability to reduce medication burden
- Reduction in hospitalizations for movement disorder crises
- Therapy that can be adjusted or turned off if needed
Improvement with DBS typically happens gradually over weeks to months as stimulation settings are adjusted.
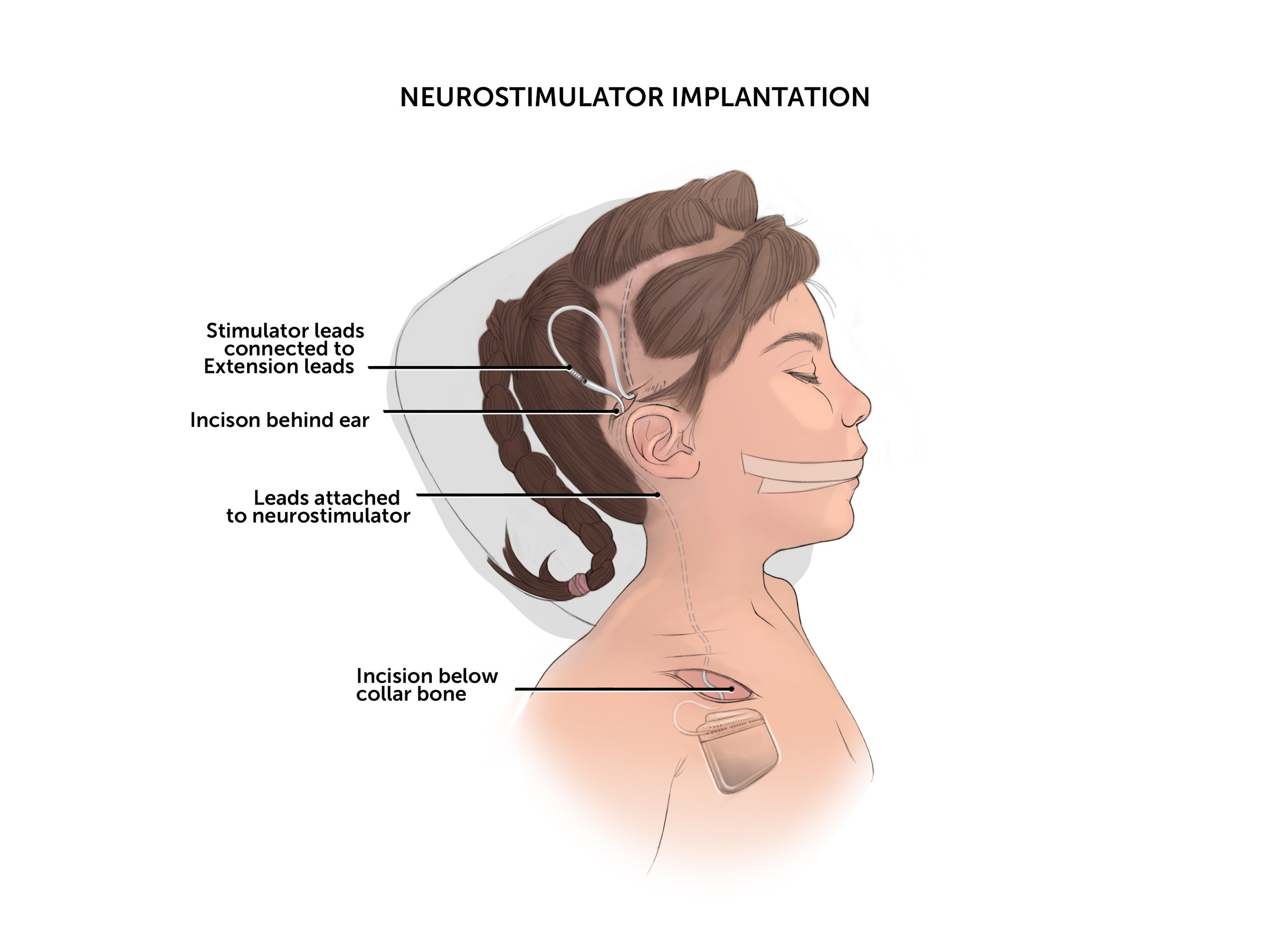
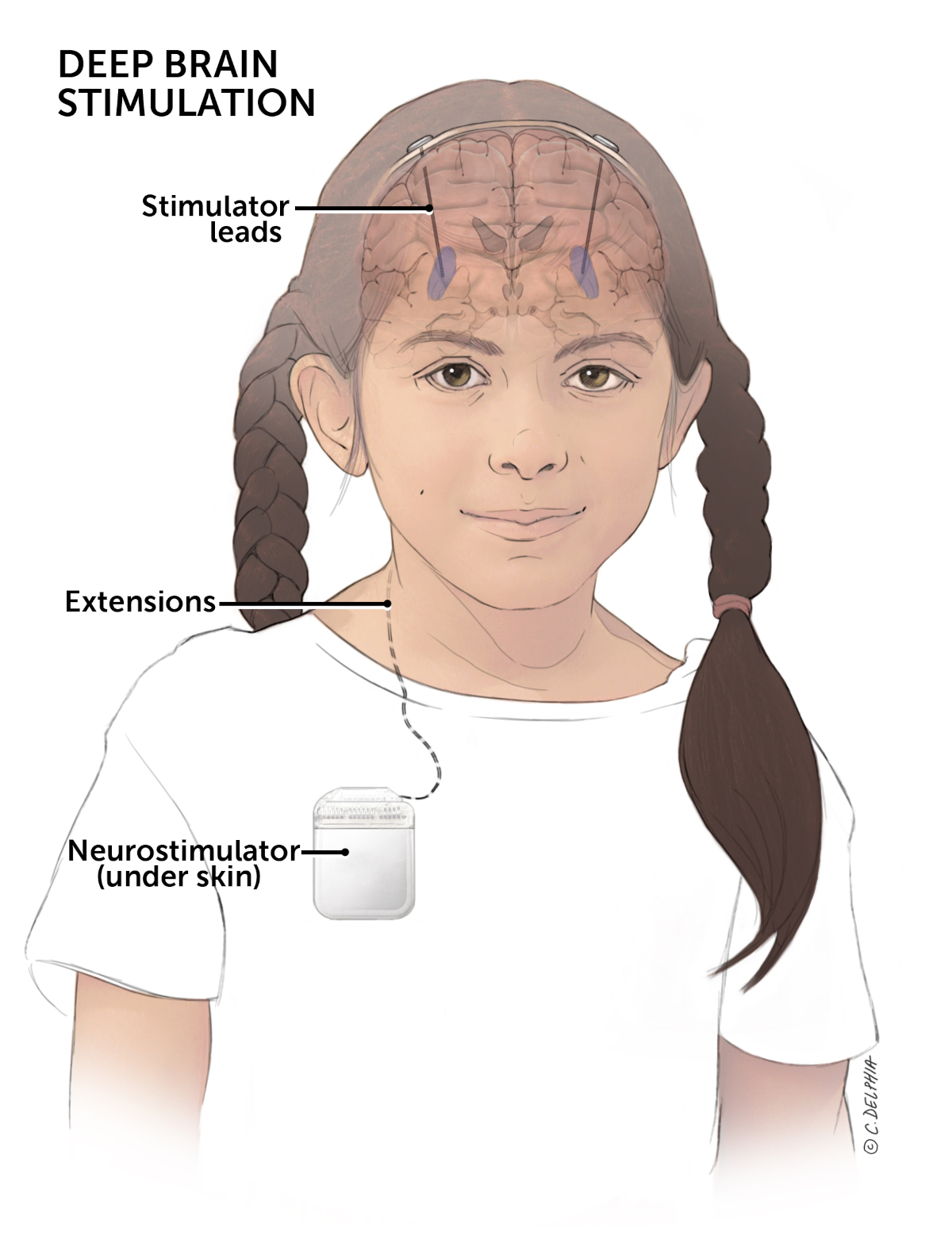
A DBS system includes:
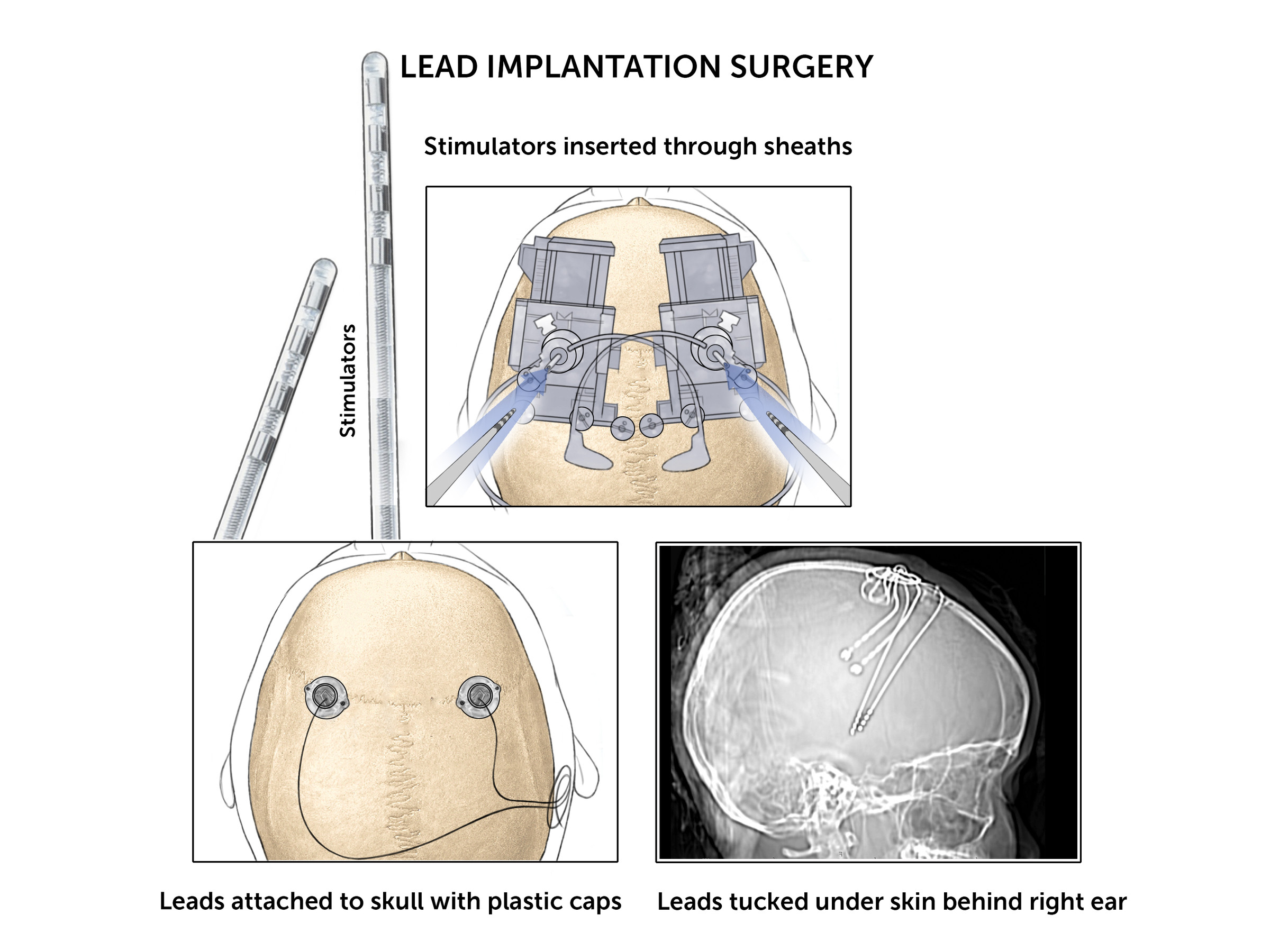
- Thin wires (leads) implanted in specific regions of the brain
- Extension wires tunneled under the skin
- A neurostimulator, usually implanted under the skin just below the collarbone
For children with movement disorders, electrodes are generally placed in the globus pallidus internus (GPi), a part of the brain that helps control movement. After surgery, stimulation settings — such as intensity, pulse width, and frequency — are customized and adjusted over time to maximize benefit and comfort.
What to expect during deep brain stimulation
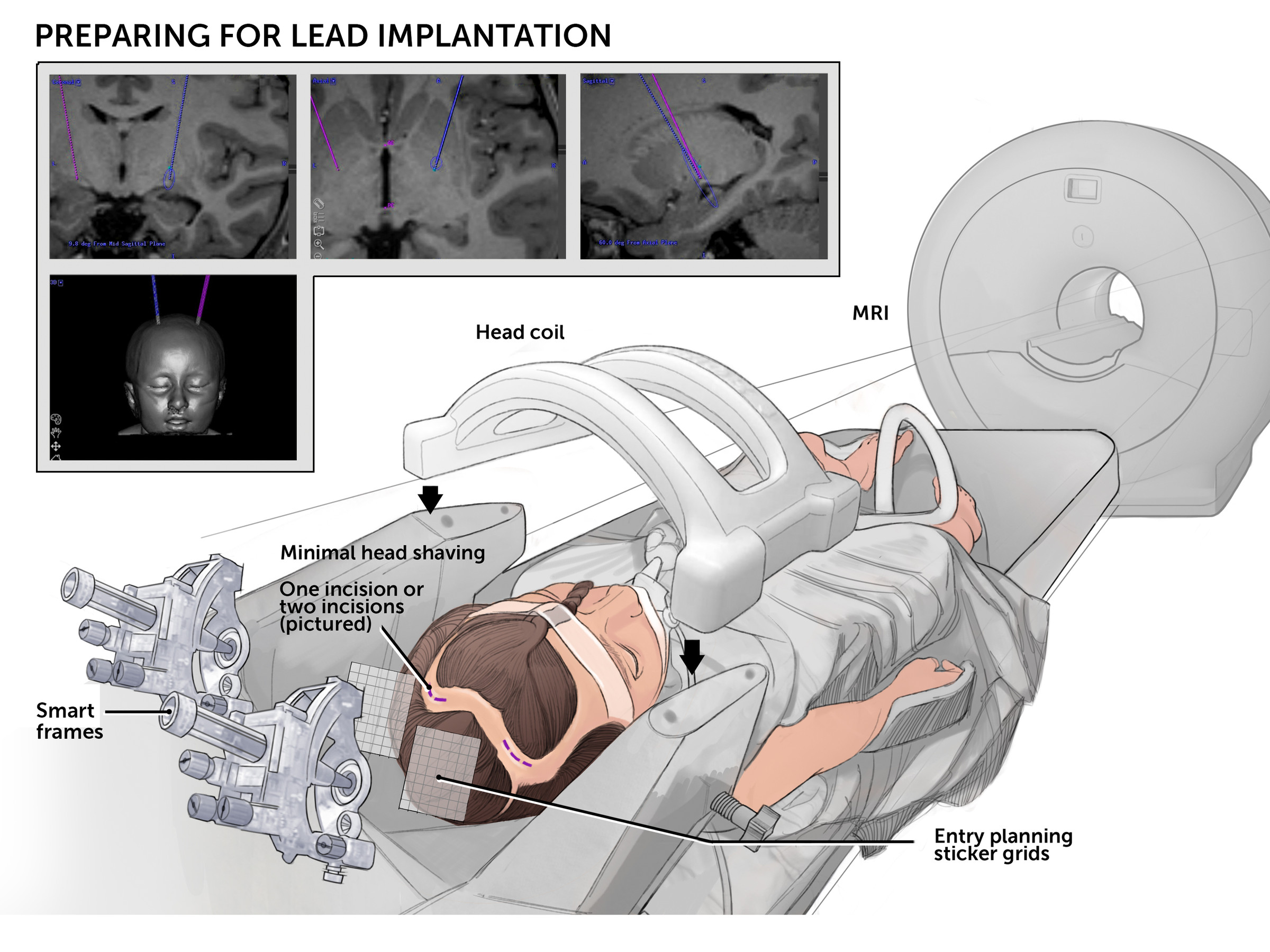
Pre-operative evaluation
Before DBS, children are evaluated by our multidisciplinary team, which may include:
- Pediatric neurologists specializing in movement disorders
- Pediatric neurosurgeons
- Neurogenetics specialists
- Physical medicine and rehabilitation specialists
- Psychiatry
- Physical, occupational, and speech therapists
Advanced imaging and diagnostic testing help determine whether DBS is likely to be beneficial and to help guide surgical planning.
DBS surgery
The procedure is typically performed in one stage. This involves:
- The placement of electrodes implanted in targeted areas of the brain
- The placement of a neurostimulator under the skin, either in the chest or abdomen area
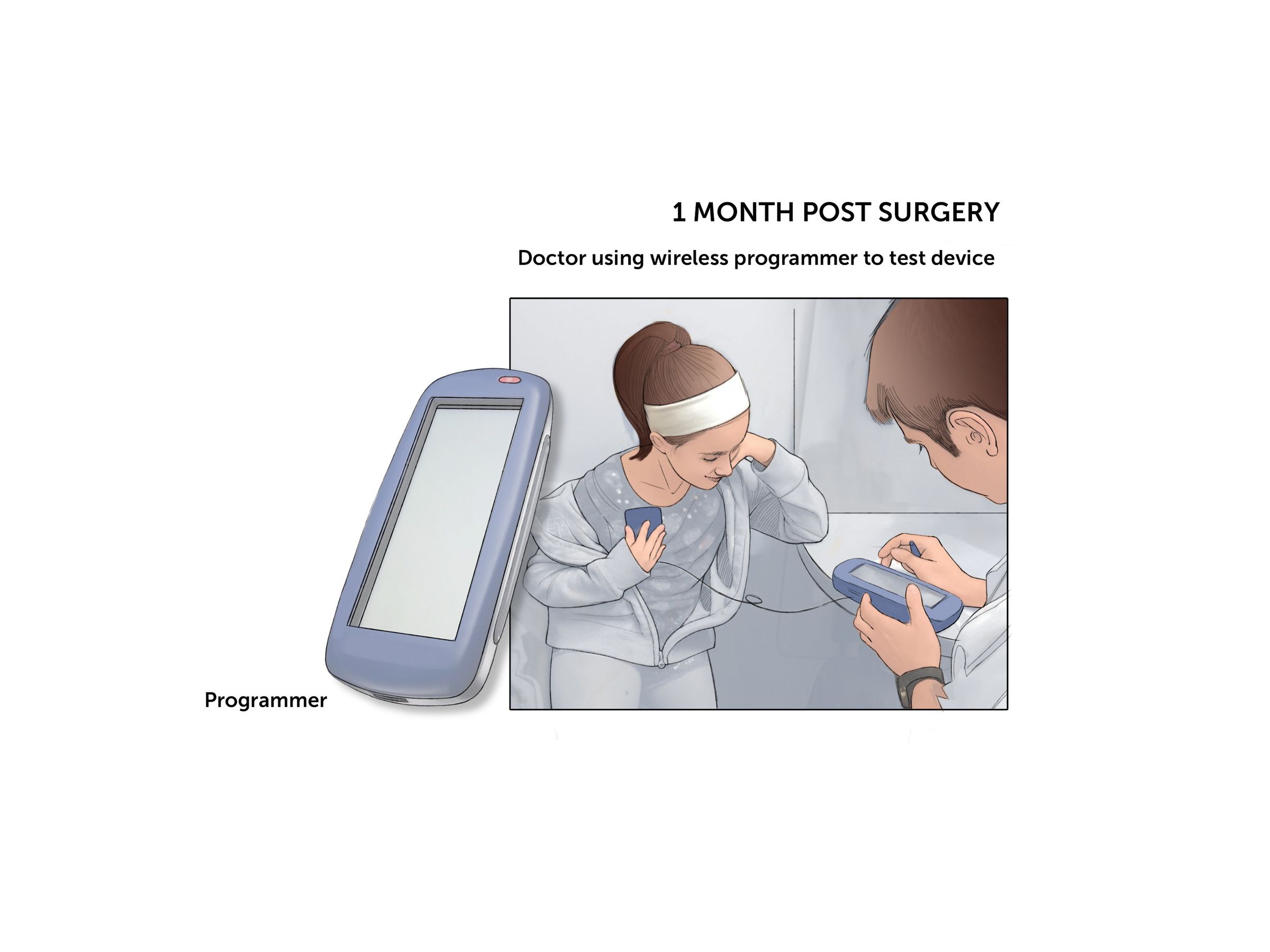
Post-op, there is an in-hospital stay for surgical recovery followed by initial programming performed in an outpatient setting.
The DBS device can be programmed and adjusted using a wireless controller. Families also receive a monitoring device to use at home.
Recovery and long-term care
After surgery, children are closely monitored with regular follow-up by our team. DBS therapy requires periodic visits to adjust stimulation settings as the child grows and symptoms change, helping ensure the best possible benefit.
Frequently asked questions
Children with significant movement symptoms may benefit from DBS. Because indications for DBS continue to expand, our team evaluates every child individually, recognizing that DBS may help different children in different ways.
DBS is generally considered a lower-risk procedure, but as with any surgery, there are potential risks. These may include:
- Common, temporary effects such as a headache or nausea after surgery
- Surgical risks such as infection or bleeding
- Issues with the device or hardware
Your child should not feel the stimulation once the settings are optimized.
Battery life depends on the stimulation settings and the type of device. Current rechargeable systems last many years.
Yes, DBS is adjustable and reversible.
For clinicians
Referring a patient
We welcome referrals for children with genetic or complex movement disorders who may be candidates for DBS. Please contact the Movement Disorders Program to discuss eligibility and required records.
DBSMatchMaker
We developed DBSMatchmaker.com for specialists caring for children with monogenic movement disorders who are considering or implanting DBS. This online platform supports peer-to-peer collaboration, shared learning, and data-informed decision-making in rare and complex cases.
Research
Publications from Boston Children’s
- Stone SS; Northam WT; Yang K; Ebrahimi-Fakhari D; et al. Bilateral globus pallidus deep brain stimulation improves motor function in ADCY5-related disorder. Mov Disord 2026 Jan 24. doi: 10.1002/mds.70181.
- Rong J; Bernardi K; Ebrahimi-Fakhari D; Yang K. DBSMatchMaker: global uptake and insights from the first year of a collaborative deep brain stimulation platform. Mov Disord 2026 Jan 8. doi: 10.1002/mds.70180.
- Yang K; Ebrahimi-Fakhari D; et al. Response to GPi-DBS in a case of EIF2AK2-associated early-onset generalized dystonia. Mov Disord Clin Pract. 2025 Oct 11. doi: 10.1002/mdc3.70395.
- Ebrahimi-Fakhari D; Yang K; Stone SS; Northam W; et al. Surgical complications of deep brain stimulation in children across targets and indications: multicenter analysis of the CHILD-DBS registry. Neurology. 2025 Nov 11;105(9):e214201. doi: 10.1212/WNL.0000000000214201. Epub 2025 Oct 10.
- Yang K; Ebrahimi-Fakhari D; et al. DBSMatchMaker: connecting clinicians globally for deep brain stimulation in rare diseases. Mov Disord. 2025 Apr;40(4):765–767. doi: 10.1002/mds.30131.
- Zaman Z; Stone SS; Northam WT; Ebrahimi-Fakhari D; et al. Deep brain stimulation for medically refractory status dystonicus in UBA5-related disorder. Mov Disord. 2023 Sep;38(9):1757–1759. doi: 10.1002/mds.29428. Epub 2023 May 2.
- Stone SS; Alterman RL. Deep brain stimulation for dystonia. In: Youmans JR, Winn HR, editors. Youmans Neurological Surgery-7th edition. Philadelphia: Saunders/Elsevier; 2015.